Histamine intolerance is based on the imbalance between the accumulation of histamines and the necessary degradation of the substance. Histamines are messenger substances produced naturally in the body but are also taken up through many foods.
If histamines are released in the body in excessive amounts or are not broken down sufficiently, this leads to defective regulation of numerous bodily functions. Typical symptoms include complaints such as digestive problems, headaches and skin irritations.
Those affected often find it difficult to identify the triggers of the allergy-like symptoms and to recognize a possible connection. We will give you an overview of the most important questions and answers regarding the topic of histamine intolerance.
What are histamines and what role do they play in our bodies?
How does a histamine intolerance manifest itself?
What does the treatment for a histamine intolerance look like?
Which foods contain a lot of histamines?
Histamines: a messenger substance with far-reaching functions
Chemically, histamines belong to the biogenic amines. They occur in small amounts in numerous foods and are formed during the breakdown and conversion of proteins. At the same time, histamines are produced in the body as a tissue hormone (messenger substance, mediator).
When histamines are released by the body, muscles contract and blood vessels relax in the affected areas. Histamines play an important role in allergic reactions, infections and inflammations.
Histamines put the body on alert and influence, for example, the secretion of gastric acid, the regulation of blood vessels and the development of nausea and vomiting. Furthermore, histamines act as neurotransmitters and influence our sleep-wake state, intestinal movements, appetite control, learning ability and many other functions.
Our body produces histamines itself and stores them in mast cells, for example. If necessary, they are released abruptly and lead to the typical symptoms of allergic reactions.
At the same time, histamines are absorbed through food. They are present in varying concentrations in both animal and plant foods.
Histamine intolerance: causes
A histamine intolerance describes the reaction of the body’s intolerance to an increased amount of histamines. Histamines are stored in various cells (such as mast cells and nerve cells) and released by stimuli.
These stimuli include:
- The body’s own enzymes,
- Various drugs (such as X-ray contrast media, muscle relaxants, acetylsalicylic acid),
- Food,
- Inflammations and diseases (such as intestinal diseases, hives, chronic kidney failure) and/or
- physical stimuli (such as injuries or a lack of oxygen).
Those affected by a histamine intolerance have more histamines in their body than can be broken down. The critical threshold value of histamines varies from person to person. If it is exceeded, the characteristic complaints and symptoms occur.
According to scientists and physicians, such a disturbed histamine degradation can have various causes. Our body basically has two enzymes that are able to break down histamines:
- Diaminooxidase (DAO): The enzyme diaminooxidase breaks down histamines outside the cells (for example, in the blood).
- Histamine N-methyl transferase: The enzyme histamine N-methyl transferase deactivates histamines directly inside the cell.
If one or both enzymes are deficient or have a disordered function, histamines can no longer be broken down sufficiently. The consequence is histamine intolerance.
Overall, histamine intolerance is a controversial disease. The form and severity of the symptoms vary greatly from patient to patient. They also apply to a large number of other diseases, which makes a clear diagnosis difficult.
According to medical experts, about one percent of people in Germany are affected by histamine intolerance – 80 % of them are women. The intolerance often begins in middle age.
Histamine intolerance: symptoms
The symptoms of histamine intolerance vary in form and severity. Some patients show only isolated symptoms, while in other patients several functions and areas of the body are affected.
Symptoms of intolerance:
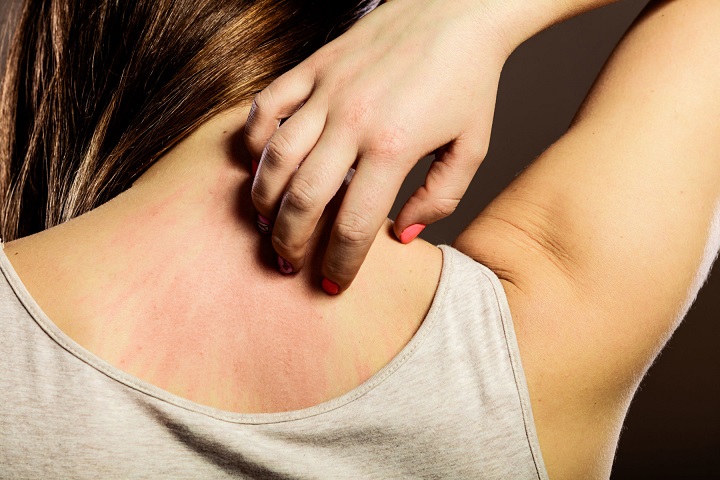
- Skin: hives, itching, reddened and warm areas of skin
- Brain: headache, migraine, dizziness, nausea, vomiting, fatigue, reduced attention
- Cardiovascular system: racing heart, palpitations, falling blood pressure
- Gastrointestinal tract: abdominal pain, cramps, diarrhea, flatulence
- Respiratory tract: runny or blocked nose, shortness of breath
Histamine intolerance: diagnosis and treatment
A clear diagnosis of histamine intolerance is not yet possible. Often, after a detailed discussion with the patient, doctors initially rule out other causes for the symptoms. These include, for example, gastrointestinal diseases or a lactose or fructose intolerance.
Doctors recommend a comprehensive change of diet or a targeted provocation test under medical supervision to test the tolerance level of the affected person.
The treatment of a histamine intolerance usually involves avoiding the triggering factors. An adapted diet promises the best chances of treatment. Food and beverages with a high histamine content are avoided.
Nutritional tips for histamine intolerance
In principle, the longer food is stored or matured, the higher its histamine content. People with histamine intolerance should pay special attention to fresh and unprocessed foods.
There are three food groups that people with histamine intolerance should know and avoid
Foods with a high histamine content
The content of histamine or its precursor histidine is additionally increased by maturing and fermentation processes. Therefore, some examples of unfavorable foods are mature cheeses, alcohol, sauerkraut and smoked sausages.
Examples of foods rich in histamines:
- Fish (such as mackerel, herring, tuna),
- Cheese (like Gouda, Camembert, Parmesan),
- Meat (sausage, salami),
- Vegetables (spinach, eggplant, tomatoes),
- Alcohol (wine, beer, champagne),
- Vinegar and
- Yeast products.
Food containing other biogenic amines
The enzyme diaminooxidase (DAO) is not only responsible for the degradation of histamines, but also other biogenic amines, such as tyramine, serotonin, spermine, cadaverine. If a large number of other biogenic amines are present, it is possible that even small amounts of histamines are no longer broken down.
The following foods contain numerous biogenic amines and should be avoided:
- Peanuts,
- Wheat germ,
- Various types of fruit (such as pineapple, kiwi, bananas, pears, raspberries) and
- Legumes (such as lentils, beans and soya).
Foods that release histamines
Foods that ensure that the body’s own stored histamines are released are called histamine liberators. These should also be avoided as far as possible in case of histamine intolerance in order to prevent inflammation.
These include, for example:
- Citrus fruits,
- Alcohol,
- Chocolate and cocoa,
- Tomatoes and products made from them (such as ketchup and tomato juice),
- Seafood and
- Nuts (especially walnuts and cashew nuts).
Histamine intolerance as a cause of psoriasis
The reduced breakdown of histamines often leads to unpleasant skin problems such as hives, reddened skin and itching.
Is there possibly also a connection with the chronic inflammatory skin disease psoriasis?
To date, there is no conclusive evidence that intolerance to histamines is a possible cause or trigger of psoriasis. Doctors and scientists always emphasize that every affected person has his or her own psoriasis and therefore has to pay individual attention to his or her personal triggering factors.
Doctors are certain that the gastrointestinal tract, our diet as a whole and individual foods have an influence on the severity and course of psoriasis disease. To what extent a histamine intolerance also contributes to psoriasis is still unclear.
However, patients with psoriasis often report that the consumption of foods rich in histamines leads to a worsening of their psoriasis.
As is often the case, the only thing that helps in this case is to consciously avoid individual triggers in the form of histamine-rich foods and consequently to check whether an improvement of the symptoms can be seen.
Histamine intolerance: an intolerance that often leads to skin problems
Histamine intolerance is not yet considered a “real” disease by many doctors. Those affected, however, see it differently. The physical consequences of histamine intolerance are not only unpleasant, but also far-reaching. In the absence of a diagnosis, histamine intolerance can lead to painful and persistent symptoms.
The right diet can bring about prompt improvement. If affected persons refrain from eating histamine-rich foods during treatment (as much as possible), the symptoms usually subside quickly. You can also talk to your doctor so that he can prescribe a better-tolerated medication if you suffer from a histamine intolerance.
Your doctor can also prescribe a better-tolerated preparation for medication that may trigger a histamine intolerance.
Have you ever thought about histamine intolerance? Do the symptoms look familiar? Share your experiences with other people affected by histamine intolerance in our Facebook group – we look forward to seeing you!
Histamine intolerance FAQ
Which foods contain a lot of histamines?
Foods with a particularly high content of histamines are fish, cheeses, meats, vegetables and yeast products. People affected should also avoid alcohol and products with a high proportion of vinegar. Ripening, maturing and fermentation processes also increase the histamine content. Mature cheeses, sauerkraut, smoked sausages and wine products should therefore be avoided by people with a histamine intolerance.
How does a histamine intolerance manifest itself?
Depending on the personal limit of the histamine intolerance, the form and degree of incompatibility varies from patient to patient. The most common symptoms of histamine intolerance include skin complaints such as hives, itching, reddening and warming of the skin. Often the gastrointestinal tract is also affected in the form of abdominal pain, cramps, diarrhea and flatulence. In addition, symptoms such as headaches, migraines, fatigue, palpitations and a blocked nose can also occur.
What happens if there are too many histamines?
If our body cannot break down the histamine produced by itself or supplied through food to a sufficient extent, the typical symptoms of an allergic reaction occur. The histamines put the entire body on alert and influence, for example, the regulation of blood vessels, the secretion of gastric acid and intestinal movements. A blocked nose, nausea and vomiting, as well as itching and reddening of the skin, are common symptoms.
Click here to see all sources
Sources:
Chung B.Y., Cho S.I., Ahn I.S., Lee H.B., Kim H.O., Park C.W., Lee C.H. (2011): “Treatment of Atopic Dermatitis with a Low-histamine Diet”, in: Annals of Dermatology. URL: https://www.ncbi.nlm.nih.gov/pubmed/22028584 (accessed on 23.10.2019)
Fritzsche D.: „Histamin-Intoleranz“, Gräfe und Unzer Verlag, 2012
Kim S.H., Kang Y.M., Kim S.H., Cho B.Y., Ye Y.M., Hur G.Y., Park H.S. (2009): “Histamine N-methyltransferase 939A>G polymorphism affects mRNA stability in patients with acetylsalicylic acid-intolerant chronic urticaria”, in: Allergy. URL: https://www.ncbi.nlm.nih.gov/pubmed/19178400 (accessed on 23.10.2019)
Maintz L., Bieber T., Novak N. (2006): “Die verschiedenen Gesichter der Histaminintoleranz: Konsequenzen für die Praxis”, in: Deutsches Ärzteblatt. URL: https://www.aerzteblatt.de/pdf.asp?id=53958 (accessed on 23.10.2019)
Reese I. et al. (2017): „German guideline for the management of adverse reactions to ingested histamine“, in: „Allergo Journal International“. URL: https://link.springer.com/article/10.1007/s40629-017-0011-5 (accessed on 23.10.2019)
Schleip T.: „Histamin-Intoleranz: Wenn Essen krank macht“, Georg Thieme Verlag, 2010
Szczepankiewicz A., Brêborowicz A., Sobkowiak P., Popiel A. (2010): “Polymorphisms of two histamine-metabolizing enzymes genes and childhood allergic asthma: a case control study”, in: Clinical and Molecular Allergy. URL: https://www.ncbi.nlm.nih.gov/pubmed/21040557 (accessed on 23.10.2019)

Bernd is one of the founders of Simply Psoriasis. He has been suffering from psoriasis for more than 20 years, but sees the chronic skin disease with more composure than a few years ago (which was a hard work). Nevertheless, he is very keen to make psoriasis easier and more socially accepted.







Last Comments