In medicine, plaques refer to a spot-shaped, often slightly raised change. In the field of dermatology, it is a matter of extensive skin changes, such as chronic inflammatory psoriasis (plaque psoriasis).
We explain what a plaque is, how it develops and how plaques are treated in the context of psoriasis.
What’s a plaque?
The term plaque originally comes from the French and means plate or stain.
Plaques are the most obvious symptom of psoriasis vulgaris, which for this very reason is also called plaque psoriasis. This form of psoriasis is the most common form of psoriasis with about 85%.
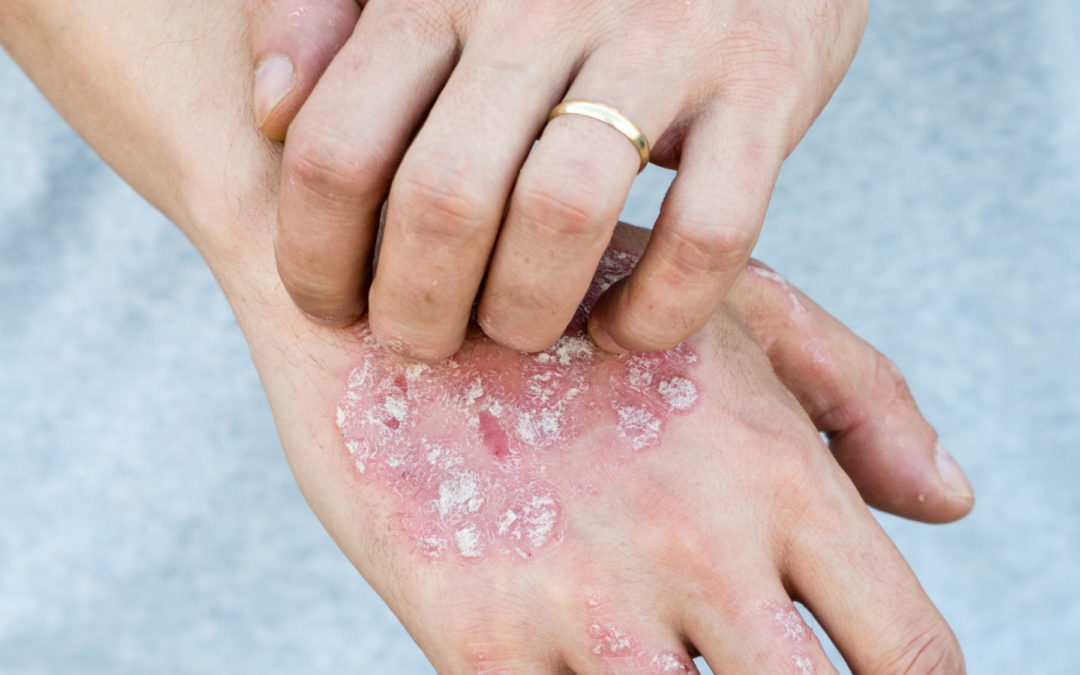
Plaques are usually coin- to palm-sized spots, which are sharply defined, reddened and usually slightly raised on the skin. In the case of psoriasis vulgaris, these skin changes are often found in the following places:
How does a plaque develop?
In the chronic inflammatory skin disease psoriasis, the body’s own immune system causes inflammation by attacking healthy, endogenous tissue. These inflamed skin areas are covered with silvery white scales.
This formation of body scales is caused by an excessive production of new skin cells on the upper layer of skin (epidermis). In healthy people, skin cells need about 25 to 27 days for skin renewal, whereas those affected by psoriasis need only five to seven days. This overproduction of skin cells leads to thickening at the inflamed areas, as neighbouring skin cells push over each other and stick together.
Most commonly affected are the extensor sides of the extremities, such as elbows and knees, and the hairy scalp (psoriasis capitis). Plaques are accompanied by severe itching, burning and painful skin tears in about 70 percent of those affected.
What is psoriasis (plaque psoriasis)?
Psoriasis is a chronic inflammatory skin disease that is still not curable, but can be treated well. The most common form of psoriasis is psoriasis vulgaris (plaque psoriasis), which accounts for about 85 percent of all cases.
Other forms of psoriasis are for example:
- psoriasis guttata (special form for children),
- psoriasis capitis (psoriasis of the scalp),
psoriasis of the nails (psoriasis of the nails), - psoriatic arthritis (chronic inflammatory disease of the joints with skin involvement),
- psoriasis pustulosa (psoriasis with pustule) or
- psoriasis inversa (psoriasis in skin folds and body bends).
Psoriasis causes
To date, the causes of psoriasis are not fully understood. However, it seems certain that it is a combination of two components.
On the one hand, scientists and physicians consider a genetic predisposition to be very likely. This does not necessarily mean that psoriasis is inherited, but it does mean that the tendency to get psoriasis is genetically passed on.
On the other hand, triggers are often responsible for the outbreak of psoriasis. Known triggers of psoriasis vulgaris are for example various infections, stress, injuries and certain medications.
Psoriasis treatment
Psoriasis vulgaris is not curable, but is now well treatable. Dermatology offers various treatment approaches for this. Together with your dermatologist it is important to find the most promising therapy according to the form and severity of the psoriasis.
Local therapy using creams, ointments, lotions, bath additives and shampoos is basically used for all forms of psoriasis vulgaris. In addition, light therapy in the form of sunlight or infrared rays or even laser therapy can provide relief.
In the case of moderate to severe forms, systemic therapy using drugs such as methotrexate, fumaric acid esters or biologicals is often used.
Living with psoriasis
Everyone has their own psoriasis – the form and severity of this skin disease is individual as well as the course and necessary therapy. However, physicians and patients themselves name the following factors of a healthy lifestyle that lead to an improvement of psoriasis:
- healthy and balanced diet,
- sufficient physical exercise,
- abstention from alcohol and cigarettes and
- reduction of stress (for example through yoga or autogenic training).
Plaques – the obvious and distressing symptoms of psoriasis
As a chronic inflammatory skin disease, psoriasis in any form and expression is in itself a burden for those affected. In addition, many of the patients feel a great sense of shame, triggered by the various symptoms of psoriasis.
The sharply defined, reddish and raised foci of psoriasis vulgaris are covered with dense, silvery white scales. Those affected are often afraid of the reactions of their fellow human beings, not least because ignorant people mistakenly believe that plaques are a sign of an infectious disease.
Everyday things, such as a visit to the hairdresser, are often a stressful and frightening challenge for those affected.
Sharing feelings, experiences and practical problems with other patients can be a great help. Our Facebook group is the ideal platform for this – we look forward to seeing you!
FAQ on plaque
What is a plaque?
Doctors refer to coin-sized to palm-sized spots in skin diseases such as psoriasis vulgaris as plaques, which are sharply defined, reddened and slightly raised on the affected skin areas. The name plaque is the French term for plate or stain. In the chronic inflammatory skin disease psoriasis vulgaris, plaques frequently occurs on the elbows, back, knees, ears and scalp.
How dangerous is psoriasis?
Psoriasis is a skin disease that progresses in relapses and is still not curable, but can be treated well. At around 85%, psoriasis vulgaris is the most common form of psoriasis. Nowadays, medicine offers sufferers numerous and good treatment options to alleviate the symptoms. Those affected can also make a valuable contribution themselves by ensuring a healthy and conscious lifestyle and avoiding triggering factors. A balanced and targeted diet, sufficient physical exercise and conscious reduction of stress are helpful factors in the treatment of psoriasis.
What is plaque formation?
The formation of plaques is based on a misguided reaction of our body, in which the immune system erroneously attacks the body's own tissue. The resulting excessive production of new skin cells on the epidermis leads to thickening of the inflamed areas, which are covered by silvery white scales. Frequently affected are the extensor sides of the extremities, such as elbows and knees, and the hairy scalp.
Click here to find all references
Sources:
Boehncke W.H., Schön M.P. (2015): „Psoriasis“, in: Lancet. URL: https://www.ncbi.nlm.nih.gov/pubmed/26025581 (Zugriff am 03.11.2019)
Luba K.M., Stulberg D.L. (2006): „Chronic plaque psoriasis“, in: American Family Physician. URL: https://www.ncbi.nlm.nih.gov/pubmed/16506705 (Zugriff am 03.11.2019)
Reich K., Krüger K., Mössner R., Augustin M. (2009): „Epidemiology and clinical pattern of psoriatic arthritis in Germany: a prospective interdisciplinary epidemiological study of 1511 patients with plaque-type psoriasis“, in: The British Journal of Dermatology. URL: https://www.ncbi.nlm.nih.gov/pubmed/19210498 (Zugriff am 03.11.2019)
Strand V., Gonçalves J., Hickling T.P., Jones H.E., Marshall L., Isaacs J.D. (2019): „Immunogenicity of Biosimilars for Rheumatic Diseases, Plaque Psoriasis, and Inflammatory Bowel Disease: A Review from Clinical Trials and Regulatory Documents“, in: BioDrugs. URL: https://www.ncbi.nlm.nih.gov/pubmed/31721107 (Zugriff am 03.11.2019)
Weigle N., McBane S. (2013): „Psoriasis“, in: American Family Physician. URL: https://www.ncbi.nlm.nih.gov/pubmed/23668525 (Zugriff am 03.11.2019)

Bernd is one of the founders of Simply Psoriasis. He has been suffering from psoriasis for more than 20 years, but sees the chronic skin disease with more composure than a few years ago (which was a hard work). Nevertheless, he is very keen to make psoriasis easier and more socially accepted.







Last Comments